AVAC is committed to helping providers navigate barriers and increase immunization rates.
Quality Measures
Quality measures are an important tool for providers to assess which vaccines a patient has had and make strong recommendations to vaccinate during a visit.
Quality measures encourage better tracking, better reporting, and increased adult immunization rates by reducing missed opportunities to vaccinate. AVAC advocates for the adoption of two immunization quality measures, the Adult Immunization Status Measure (AIS) and the Prenatal Measure.
The AIS measure is a composite of several age-recommended vaccines for adults, including influenza; tetanus and diphtheria (Td) or tetanus, diphtheria, and acellular pertussis (Tdap); zoster; and pneumococcal. Adoption of an AIS measure would encourage a more systematic approach for receiving recommended vaccines.
The prenatal immunization status measure includes two vaccines recommended for every pregnancy (influenza and tetanus, diphtheria toxoids, and acellular pertussis (Tdap). Using this quality measure widely will improve the likelihood of pregnant women being assessed and immunized at provider encounters.

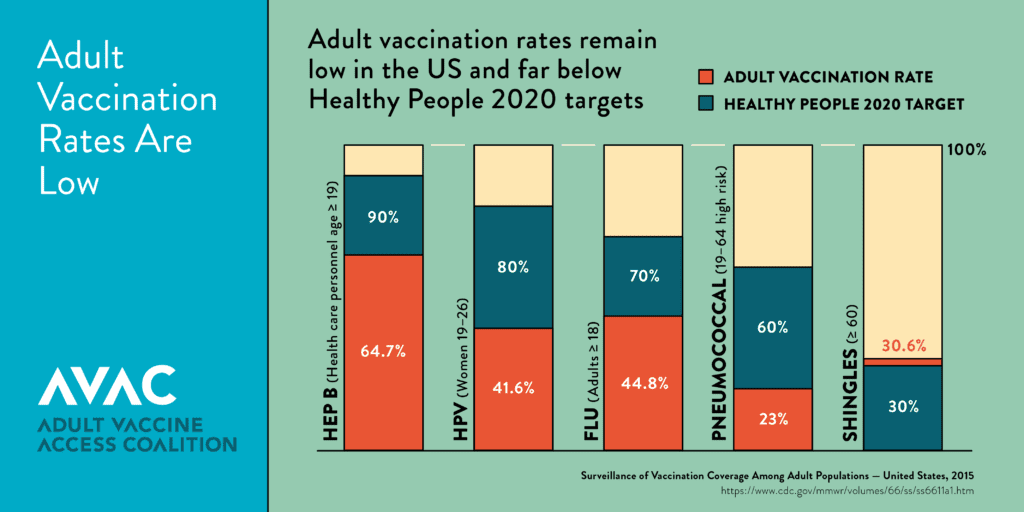
Many adults are not being assessed and offered recommended vaccines, resulting in poor immunization coverage rates nationally.
AVAC Member
AVAC’s work to support quality measures includes:
• Ensuring HP2030 operationalizes adult immunization metrics.
• Working with CMS to adopt AIS/prenatal composite measures in Medicare and Medicaid.
Supporting Providers
AVAC is committed to supporting providers that are critical for increasing rates, including improving reimbursement rates for recommending and administering vaccines.
Providers face barriers in providing adult vaccination, including low reimbursement, delays in receiving payment, and expenses around stocking vaccines. Together, these factors have driven many providers to discontinue or limit vaccine services to patients. Providers are less likely to recommend vaccines that they do not carry.
A recommendation by their physician is one of the primary reasons why patients receive vaccines. AVAC’s regulatory work to ensure that provider immunization reimbursement policies reflect the purchase and administration costs of vaccines will encourage providers to stock, store, and recommend vaccines to their adult patients.
AVAC Member
AVAC’s work to support providers includes:
• Advocating for increased vaccine coding and administration fees.
• Advocating for timely reimbursement around vaccines.
• Improving CMS educational materials to patients and providers.